October is Breast Cancer Awareness Month. It’s time for renewed attention to the disease, which affects hundreds of thousands of American women each year.
According to the National Cancer Institute of the National Institutes of Health, women in the United States have a 1 in 8 (12.9%) chance of developing breast cancer during their lifetime, while men in the United States have a 1 in 800 ( 0.13%).
The Centers for Disease Control and Prevention (CDC) reports that approximately 264,000 women are diagnosed with breast cancer each year, and approximately 42,000 women die from the disease. (About 2,400 men are diagnosed with breast cancer each year, and about 500 men die from it each year, data from the CDC shows.)
Katie Couric’s Breast Cancer: What Other Women Can Learn From Her Diagnosis
Because breast cancer is more common in women over the age of 40, health professionals and organizations recommend regular breast cancer screenings for middle-aged and older women. This includes the mammogram, a breast cancer screening method that has led to age-based debate among experts.
There are also important breast cancer risk factors to look out for, experts say.
Breast Cancer Awareness Month is held each October.
(iStock)
Kathleen Kiernan Harnden, Ph.D., director of breast oncology at the Inova Schar Cancer Institute in Annandale, Virginia, told Fox News Digital:
Harnden said other high-risk factors include a family history of breast cancer, a known genetic mutation, or a previous breast biopsy.
Breast Cancer Survivor Inclusive Lingerie Brand Targets Diagnosed Women
That’s why Harnden says there are three questions every woman should ask herself before asking for a mammogram visit or appointment.
1. Am I at high risk for breast cancer?
2. How can I reduce my risk of breast cancer?
3. Are mammograms three dimensional (3D) or two dimensional (2D)?
Harnden recommends 3D mammography over 2D because multiple images are taken from different angles and the analysis of breast tissue can be clearer.
We will discuss these topics in detail here.
What is Breast Cancer?

According to the National Cancer Institute, about 1 in 8 women will develop breast cancer in their lifetime.
(iStock)
Breast cancer is a disease that forms in breast tissue when breast cells “change and grow out of control,” according to MedlinePlus, an online health information service created by the U.S. National Library of Medicine.
The cells that cause breast cancer usually form tumors, which are abnormal masses of tissue.
Cancer cells and cancerous tumors (malignant) can disrupt organ function and kill healthy cells if they continue to spread, according to a report by MedicalNewsToday, a medical news website owned by Healthline. ,It is dangerous. media.
According to the National Cancer Institute, breast cancer is the second most common cancer in women after skin cancer.
Breast cancer incidence in women by age group: CDC
– 15-19 years: 0.2 per 100,000 women
– 20-24 years: 1.8 per 100,000 women
– 25-29 years old: 10.5 per 100,000 women
– Age 30-34: 30.1 per 100,000 women
– Age 35-39: 64.8 per 100,000 women
– Age 40-44: 131.7 per 100,000 women
– 45–49: 201 per 100,000 women
– Age 50-54: 240.7 per 100,000 women
– 55-59 years: 273.3 per 100,000 women
– Age 60-64: 339.8 per 100,000 women
– 65-69 years: 425.2 per 100,000 women
– Age 70-74: 475.8 per 100,000 women
– 75-79 years: 466.1 per 100,000 women
– Age 80-84: 420.7 per 100,000 women
– 85+: 318.2 per 100,000 women
Breast cancer diagnosis is very rare in teenagers. According to the CDC, the incidence rate for teenage girls from age 15 to her 19 is 0.2 per 100,000 of her population.
Breast cancer incidence for girls under 15 has not been calculated. This is because the CDC suppresses data if there are fewer than 16 of her cases, which the CDC points out on his webpage for “National Cancer Statistics: Visualizing the Data.”
Breast Cancer Awareness: FOX NEWS’ Kayleigh Matheny, Jerry Willis, and Jackie D’Angelis Talk Real About Diagnosis
CDC data shows that the incidence of breast cancer increases steadily with age, but remains low in women under the age of 40.
Not all experts agree on whether women under the age of 40 should have mammograms, but incidence data released by the CDC dating back to 2019 show that women in their 20s and 30s A woman is diagnosed with breast cancer.
The incidence of breast cancer in middle-aged women increases steadily every four years.
For women aged 20 to 24, the incidence of breast cancer is 1.8 per 100,000.
The incidence jumps to 10.5 per million, 30.1 per 100,000, and 64.8 per 100,000 in women aged 25-29, 30-34, and 35-39, respectively.
Woman’s 57-pound weight loss allows her to discover breast cancer: ‘I feel lucky’
According to CDC data, the incidence of breast cancer rises sharply between the ages of 40 and 74.
The prevalence among middle-aged women increases steadily every four years. For example, women aged 40 to her 44 have a breast cancer incidence of 131.7 per 100,000 women, and women aged 55 to her 59 have a breast cancer incidence of 273.3 per 100,000 women.
Breast cancer diagnosis is even more common in older women. According to CDC data, the incidence of breast cancer in women aged 60 to 64 is 339.8 per 100,000 women, and the incidence of breast cancer in women aged 65 to 69 is 425.2 per 100,000 women. , women aged 70 to 74 have breast cancer. With an incidence of 475.8 per 100,000 women, it is the highest of any age group.
According to the CDC, the incidence of breast cancer begins to decline after age 75.
What is a Mammogram?
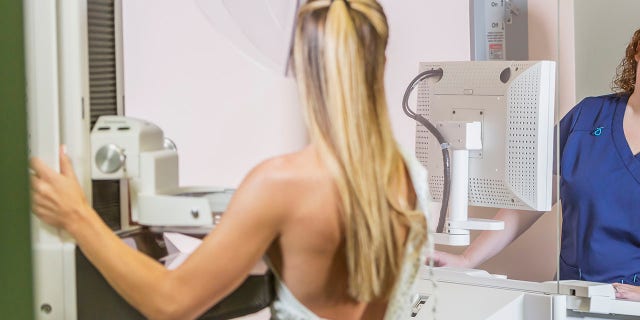
Mammography is a common breast cancer screening method that uses radiation to detect physical abnormalities in breast tissue.
(iStock)
A mammogram is an x-ray that helps doctors detect early signs of breast cancer, according to the CDC.
The machine used to perform a mammogram has a plastic plate that flattens the breast so that an x-ray image can be taken and analyzed by a radiologist for any abnormalities.
According to the CDC, mammogram results are usually reported in a few weeks.
Singer Kelly Lang on 17-year battle with breast cancer: ‘I promised God I would be a bright light for others’
Women with dense breasts are more likely to get breast cancer, health organizations report, but for women who are younger, pregnant or breastfeeding, taking hormone replacement therapy, or underweight. , some women have dense breasts.
“Dense tissue can hide cancer,” writes the CDC, “What does it mean to have dense breasts?” report.
“Fibrous and glandular tissue appears white on mammograms, as does the possibility of tumors,” the CDC continued. there is potential.”

A mammogram uses x-ray images to detect breast cancer.
(iStock)
Dr. Mona Jhaveri, a cancer researcher and founder of Music Beats Cancer, a creative nonprofit in Washington, DC, told Fox News Digital that half of women over the age of 40 have dense breast tissue. rice field.
“It’s notoriously difficult to detect cancerous lesions in women with dense breast tissue,” Jhaveri said. “Mammography is the standard of care for breast cancer screening. [but] It certainly has its risks and limitations. ”
Delaying the diagnosis of breast cancer poses a higher risk than radiation exposure.
Potential risks associated with screening mammography include overdiagnosis, false positives, anxiety, and radiation damage, according to a study published in the National Library of Medicine.
According to the U.S. Preventive Services Task Force — an independent, volunteer panel of national experts in disease prevention — women aged 40 to 49 weigh the potential benefits of mammography over potential harm.
Woman battling stage 4 breast cancer after screening delays amid pandemic
According to the CDC, similar breast screening guidelines are available from the American Cancer Society, American Medical Association, American College of Obstetricians and Gynecologists, American College of Radiological Published by the Medical Association, American Medical Association. Academy of Family Physicians.

Some mammogram machines produce 2D images and some produce 3D images.
(iStock)
Three of the six cancer organizations mentioned above recommend annual mammograms for women aged 40 to 49 who are concerned, if needed.
Women over the age of 50 are generally advised to have mammograms once every year or two.
All cancer organizations encourage women to speak with their health care providers to weigh the potential benefits and risks of having a mammogram.
Age and family history of cancer are two factors considered during a mammogram appointment, reports the CDC.
What should I know about mammogram radiation?

Mammogram machines emit radiation to create X-ray images, but this does not make the method dangerous.
(iStock)
Most breast cancer cases are diagnosed after age 50, says Jessica Shepherd, M.D., a Dallas-based obstetrician and gynecologist and chief medical officer of health information website Verywell Health. Its age marker.
“The radiation dose from a mammogram is very low and rarely poses a risk, making it a safe diagnostic tool. Mammograms are typically only needed once a year, so there is no risk of too much radiation exposure.” said Shepard. Fox news digital.
CLICK HERE TO GET THE FOX NEWS APP
She noted, “There is a small link to an increased risk of breast cancer over time. [mammogram] frequency and breast size,” but “overall, this increased risk is very small.”
Delaying the diagnosis of breast cancer poses a higher risk than radiation exposure, Dr. Shepherd said.
“If detected early, breast cancer is highly treatable, and mammograms are very beneficial in these cases,” continued Shepard. [breast cancer is] If progression is allowed, patients may have to undergo more complex treatments, such as surgery and chemotherapy, which are much more invasive than radiation exposure from a mammogram.”
Alternatives to Breast Cancer Screening
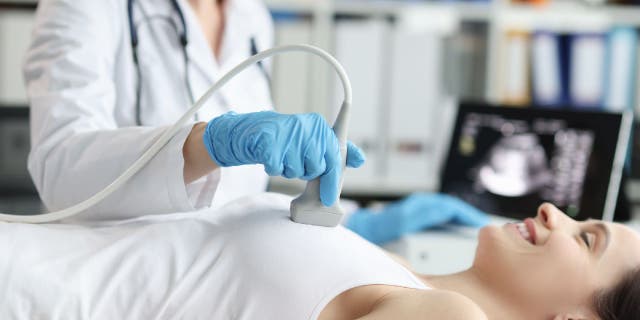
A breast ultrasound can be done to diagnose an underlying breast tumor.
(iStock)
For women who are not eligible or unwilling to have a mammogram, there are other breast cancer screening methods.
The CDC lists breast ultrasound, breast magnetic resonance imaging (MRI) clinical breast examination, and self-examination as possible screenings for breast cancer.
FOLLOW US ON FACEBOOK FOR MORE FOX LIFESTYLE NEWS
Ultrasound uses sound waves to produce images (AKA sonograms), while MRI is a computerized scan of the body that uses magnets to produce images.
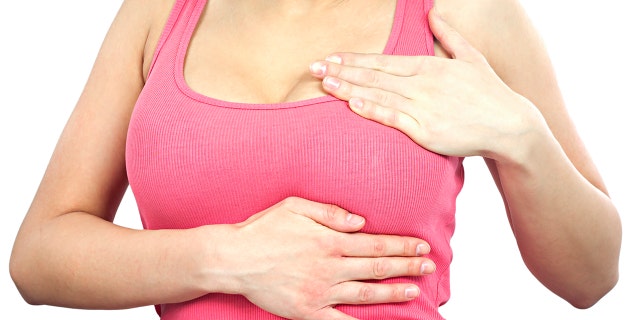
You can do a self-examination to check for early signs of breast cancer.
(iStock)
A clinical breast examination is performed by a doctor or nurse. During the exam, a medical professional will manually check the breast tissue for any abnormal lumps or other physically detectable changes.
Women can check their breasts for common breast cancer symptoms, such as lumps, pain, and changes in size.
In What Is Breast Cancer Screening, the CDC writes, “If you notice any changes, you should report them to your doctor or health care provider.” guide.
CLICK HERE TO SIGN UP FOR THE LIFESTYLE NEWSLETTER
The CDC also said, “Breast clinical examinations and breast self-exams have not been shown to reduce the risk of dying from breast cancer.

